Eczema Across the Lifespan
Reviewed by: HU Medical Review Board | Last reviewed: September 2024 | Last updated: October 2024
Atopic dermatitis, also known as eczema, is a common skin condition. It causes the skin to become red, itchy, and inflamed. This condition can affect people of all ages, from infants and toddlers to older adults. The symptoms and treatment of eczema can vary depending on the age group.1
Infants and toddlers
Atopic dermatitis often begins in infancy. About 60 percent of eczema cases develop in the first year of life. Many babies develop red, itchy patches on their skin.1,2
In infants, eczema usually appears on the:1
- Face
- Cheeks
- Forehead
- Scalp
In babies 6 to 12 months old, eczema can also appear around the:1
- Elbows
- Knees
In toddlers, eczema can appear:1
- Around the mouth
- Around the eyelids
- In the creases of the elbows and knees
- On the wrists and hands
Complications in infants and toddlers
Babies may scratch the itchy areas, leading to broken skin. This can result in infections. Keep the baby’s nails short, and consider using mittens to prevent scratching.1,2
Itching may also disrupt a baby’s sleep. Using a moisturizer before bedtime can help reduce itchiness. Taking an antihistamine like diphenhydramine (Benadryl), if recommended by your doctor, may help them sleep.1
Treatment for infants and toddlers with eczema
Eczema treatment for infants and toddlers consists of a combination of skincare and topical medicines (if needed). Here are the eczema treatment options that are recommended for babies:1,2
- Gentle skincare – Keep the baby’s skin moisturized. Use fragrance-free, hypoallergenic moisturizers. Use the “soak and seal” method: Apply moisturizer right after bathing, when the skin is still damp. Avoid long baths, as they can dry out the skin. Keep baths to 5 to 10 minutes. Use lukewarm water and mild, fragrance-free cleansers.
- Avoid triggers – Common triggers include harsh soaps, excess saliva and drooling, wool clothing, and heat. Keep the baby’s environment cool, and dress them in soft, breathable clothing.
- Medicine – If the eczema is severe, a dermatologist may prescribe mild corticosteroid creams. Use them only as directed by your doctor.
Children
As children grow, eczema may change in appearance and location. The rash may move to different areas of the body, such as:1,3
- Elbow creases
- Knee creases
- Wrists
- Neck
- Behind the ears
The skin may become thickened due to constant scratching. This is known as lichenification. Skin may also develop small bumps or become crusty.1,3
Complications in children
Many children with eczema must deal with allergies as well. In fact:3
- About one-half of kids with eczema will develop allergic asthma. Asthma symptoms include coughing, sneezing, wheezing, and chest tightness.
- About three-fourths of kids with eczema will develop allergic rhinitis or hay fever. Hay fever symptoms include itchy, watery eyes, a stuffy or runny nose, ear pressure, and fatigue.
- About one-third of kids with eczema also have 1 or more food allergies. Common food allergies include eggs, milk, peanuts, and soy.
If your child has any of the above, contact their doctor so that you can get the treatment they need. They may need to take other medicines to treat these other allergic conditions.3
Finally, visible eczema can affect a child’s self-esteem. They may feel embarrassed or anxious about their appearance. Encourage open conversations about their feelings and provide reassurance.
Treatment for children with eczema
Many treatment options exist for children with eczema, including:3,4
- Moisturizers – Use fragrance-free moisturizers regularly. This helps to keep the skin hydrated and reduces flare-ups. Use the “soak and seal” method. There are many over-the-counter (OTC) creams that are made for eczema-prone skin. Petroleum jelly (Vaseline®) is an approved eczema OTC treatment and can really lock in moisture. Moisturizers that contain ceramides help to seal in moisture as well.
- Topical creams/ointments – Dermatologists may prescribe stronger corticosteroid creams or ointments if needed. In some cases, non-steroid creams that reduce inflammation may be recommended.
- Bleach baths – Bleach baths may improve eczema by reducing inflammation and itch as well as restoring the skin barrier. Read the full instructions on bleach baths from the National Eczema Association.
- Wet wrap therapy – For severe eczema, wet wrap therapy can be helpful. After applying medicated topical cream, wrap the affected areas with damp, soft cloths. Then cover with dry clothing. This helps to soothe the skin and increase the effectiveness of the treatment.
- Education – Teach children not to scratch the affected areas. Explain the importance of applying moisturizers and medicine regularly.
- Oral medicines – Doctors also may prescribe antibiotics, immunosuppressants, biologics, and/or antihistamines, depending on how severe a child’s eczema is.
Remember that each child is different. What works for one child may not work for another. You may have to try several different treatment options before finding what works for your child. Be patient and persistent. You may need to stick with a treatment regimen for a few weeks before seeing improvement. Reach out to a dermatologist or allergist if you do not start seeing results.4
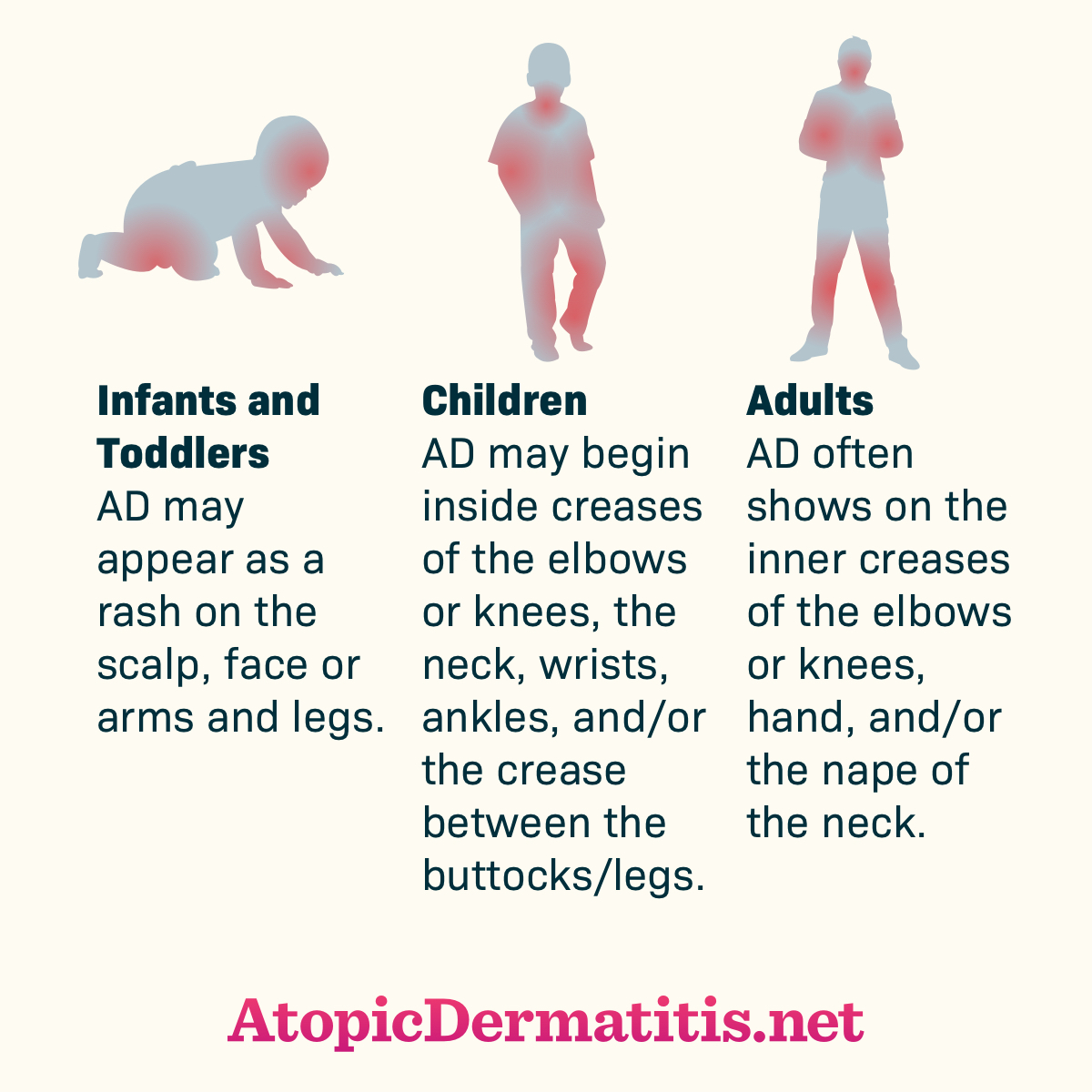
Locations of rashes from infancy to adulthood
Adults
Many children outgrow their eczema. But for some people, eczema continues into adulthood. It is also possible to develop eczema for the first time as an adult.5
Adults may experience chronic, itchy patches that are often located on the hands, feet, and around the eyes. The skin may be dry, thickened, and prone to cracking. For adults who have had eczema since childhood, eczema patches may look and feel leathery and scaly after years of intense dryness.5
Complications in adults
Some adults may have eczema complications, such as:5
- Infections
- Eye irritation or infections (if the eczema is near or on the eyelids)
- Trouble sleeping (from persistent itching)
- Poor self-esteem
- Asthma and allergies
- Contact dermatitis – a reaction of the skin when it comes into contact with certain irritants (soaps, detergents, cleaners, or other chemicals)
Treatment for adults with eczema
For adults with eczema, the following treatments are recommended:6
- Moisturize daily – Daily moisturizing is essential. Use thicker creams or ointments that provide a barrier to keep the skin hydrated.
- Avoid eczema triggers – Avoid anything that you know causes your eczema to flare, such as detergents, soaps, or other chemicals.
- Take medicines as prescribed – Dermatologists may prescribe topical steroids or other medicines to reduce inflammation. In more severe cases, oral drugs, injections, or phototherapy (light therapy) may be recommended.
- Manage stress – Stress can worsen eczema in adults. Stress can also be an eczema trigger. Techniques like meditation, regular exercise, and proper sleep can help manage stress levels.
Older adults
Eczema can also affect older adults, although it is less common. When eczema develops in older adults, it generally appears as a red rash in patches on the face, neck, and stomach/back area. Unlike in children and younger adults, eczema later in life may not be seen in the crooks of the elbows, knees, and wrists. The skin may appear thicker, but less often in the places typical of children and adults.7
Certain types of eczema are more common among the elderly, including:7
- Asteatotic eczema – a form of eczema characterized by dry, cracked, and itchy skin. It is often caused by a lack of natural oils and moisture in the skin. This type of eczema commonly occurs in older adults, especially during the winter months when the air is dry.
- Varicose eczema – a type of eczema that develops on the lower legs due to poor circulation and varicose veins. Legs can feel itchy, become swollen, and look discolored. This type of eczema often comes along with a feeling of heaviness in the legs.
Complications in older adults
As we get older, our skin becomes drier. This added dryness can make eczema patches even worse.7
In older adults, the skin is thinner and more fragile. Older adults should be mindful of skin tears and infections. Careful skin care and avoiding harsh materials or excessive friction can help prevent damage.7
Treatment for older adults with eczema
As with all adults, treatment for older people with the condition focuses on:6
- Protecting the skin from dryness with lotions and creams
- Using anti-inflammatory medicines, including cream-based corticosteroids
- Recognizing and avoiding triggers from the environment, like allergens or other chemicals
- Eating a healthy diet rich in healthy fats, protein, and zinc, which can promote healing
Moderate to severe cases of eczema in older adults often do not respond to medicated lotions or creams. Instead, strong anti-inflammatory steroid drugs taken by mouth or a biologic drug injection may be needed.